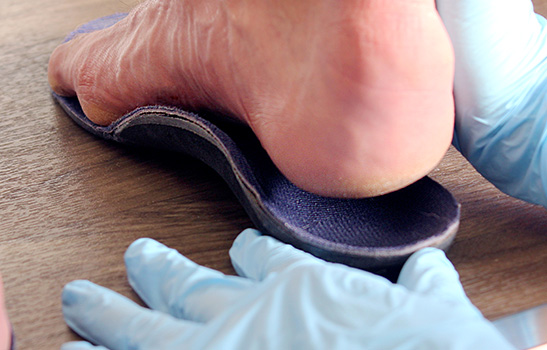
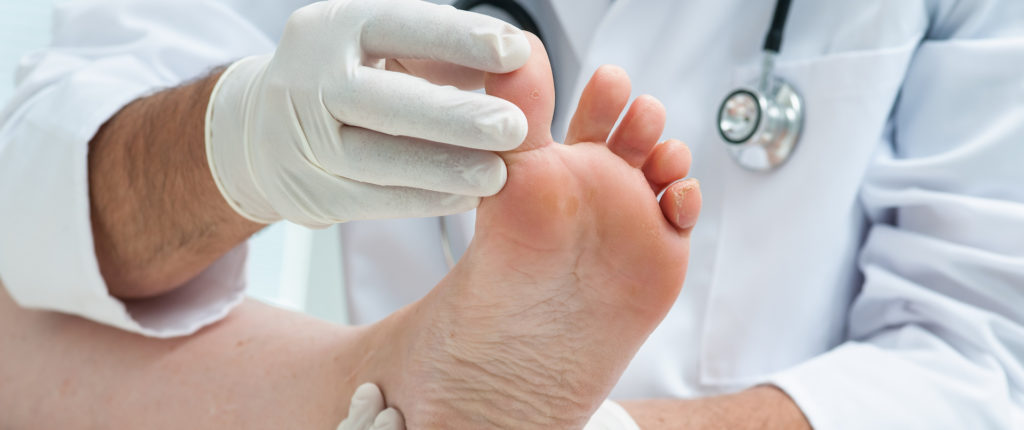
How diabetes affects feet
More than 9% of Canadians have diabetes and another 22% are pre-diabetic. This means that more than 9 million Canadians* are facing the illness! Diabetes is an insidious disease that causes a wide range of complications, many of which affect the feet. Diabetes can adversely affect your nerves, blood supply (vascularization) and immune system. This in turn can increase your risk of developing foot ulcers and requiring amputation. Some 15% to 25% of diabetics experience foot ulcers* and 85% of amputations are attributed to foot ulcers.** Fortunately, controlling blood sugar and seeing a podiatrist regularly can help prevent these outcomes, as 50% of amputations are avoidable through preventive foot care.**
* Canadian Diabetes Association: http://www.diabetes.ca/
** Wounds Canada: https://www.woundscanada.ca/
See the causes See the long term complications See how to relieve yourself at home
Signs and symptoms that diabetes affects your feet
Are you worried about diabetic foot complications? Here are some common symptoms:
- Burning sensation in feet, especially at night
- Tingling, numbness or a strange feeling on the bottom of the feet
- Poor balance or stability
- Reduced sensation in feet (e.g., not noticing a blister or cut)
- Deformities (hammertoes, bunions, arcing)
- Stiff joints
- Thick callouses (hard, dead skin)
- Very dry skin
- Sores that don’t heal
- Poor cicatrization
- Susceptibility to infection
- Reduced hair growth
- Cold or discoloured feet
- Red rash (often on the top of feet or legs)
What causes diabete to affect your feet
Type 1 and 2 diabetes are defined by poorly controlled blood sugar levels. Insulin makes it possible for blood sugar to enter your cells; it’s like a key that opens the cells’ lock. But since diabetics don’t have enough insulin, the sugar in their blood is locked out of their other tissues. With nowhere to go, the sugar stays in their blood.
When blood sugar gets too high, it becomes toxic and can attach to tissues such as arteries and nerves, especially small ones like those in your feet. This is called glycosylation. It leads to constricted blood vessels and reduced nerve conduction.
How diabete affects your nerves
When your nerves are affected (diabetic neuropathy), you can lose sensation and stop feeling pain. Even though most people think of pain as a bad thing, it’s essential for letting us know when there is a problem. In diabetics, this natural “alarm system” can stop working properly, leaving you unaware of sores that require attention.
Nerves also play a role in maintaining muscle tone. Foot muscles that don’t receive nerve signals tend to atrophy, creating an unstable environment for your bones and joints. This cause deformities such as high arches, bunions and hammertoes.
Finally, nerves help keep your skin healthy. Neuropathy can make your skin become dry, fragile and calloused.
How diabete affects your arteries
Proper circulation is needed to supply foot tissues with nutrients, oxygen, immune cells and metabolites for healing and eliminating waste products. When artery walls are damaged by diabetes, foot tissue vitality may be compromised.
How biabete affects your immune system
High blood sugar can negatively impact your immune system, making it harder for you to fight off bacterial and fungal infections. This problem is aggravated by poor circulation, as this prevents infection-fighting cells from reaching the area. That’s why people with diabetes are more prone to infection.
Progression and consequences of diabete
Since diabetes affects your nerves, arteries and immune system, it can lead to serious foot complications. This is especially true if you’ve had the disease for several years and your blood sugar levels aren’t well controlled.
Diabetics who don’t receive proper treatment often experience progressive foot trouble :
- First, nerve damage leads to changes in gait and balance. This can alter pressure distribution and cause deformities.
- If there is too much pressure or friction on specific points, the patient may develop corns and calluses.
- Due to their compromised “internal alarm system,” the patient may not notice the callus and continue walking on it, causing a blister.
- Pressure causes the skin to break, leaving a wound that gets deeper and deeper.
- Some wounds don’t heal and become chronic ulcers.
- Diabetic foot ulcers are susceptible to infection.
- If the infection becomes serious and spreads to the bone or if the patient develops gangrene due to poor circulation, the extremity may need to be amputated.
With proper care, this domino effect can often be stopped at almost any stage.
How to relieve diabetic effects on your feet
Preventive care :
- Wash feet and toes with mild soap and dry them thoroughly, especially between your toes.
- Apply moisturizer every day, but not between the toes.
- Avoid soaking your feet for more than 10 minutes.
- Check your feet daily, using a mirror if necessary. Look for redness, cuts, blisters, discolored areas or new calluses. If you can’t get a good look at your feet, ask someone for help.
- If you notice a wound, disinfect it right away and apply a bandage with Polysporin. See a doctor as soon as possible if you notice redness, swelling, hot spots, odours or pus.
How to diagnose diabete
Diabetes can be diagnosed by your family doctor or endocrinologist
What can my podiatrist do about diabetic effects on yout feet
1. Diabetic foot care :
- Diabetics should receive a medical foot care 1 to 6 times per year, depending on their overall health and the condition of their feet. Regular appointments will allow your podiatrist to monitor your condition and either prevent or respond to diabetic foot complications.
- Removing calluses can prevent the formation of pressure points that cause cracks, blisters or wounds.
- Cutting and thinning nails is important, as thick nails can lead to sores. Ingrown or infected nails must also be prevented.
- Your podiatrist may prescribe creams or medications for your skin and nails.
2. Neurological tests :
- It is important to test diabetics for foot sensitivity to determine their risk of developing complications. Preventive measures may be recommended, depending on your condition.
- These tests detect if nerves are starting to have damage.
- Initially, patients often notice a decreased ability to feel vibrations. We use a special device called a biothesiometer to quantify your ability to detect vibrations. It provides accurate readings so that we can monitor and follow your foot nerve health.
3. Vascular tests :
- It’s very important to test the blood flow in your feet, particularly since 60% of patients with peripheral arterial disease are asymptomatic.
- To quantify how much blood gets to your feet, we calculate the ratio between the pressure in your arm and in your ankle (ankle-brachial pressure index).
- We can also quantify how much blood gets to your toes by calculating the same ratio with the pressure in your big toe (toe-brachial index).
- This simple test helps us determine whether treatment is needed to prevent foot ulcers, gangrene and amputation.
4. Biomechanical exam :
- Biomechanical exams involve assessing foot function, gait and posture to detect deformities, changes in balance and poor pressure distribution, which could lead to foot health problems.
5. Plantar orthotics :
- Orthotics are very helpful in preventing diabetic foot ulcers. They ensure pressure is distributed more evenly across your foot and provide additional stability. Special materials are sometimes added to optimize the way you walk.
6. Diabetic foot ulcer care :
- First, your podiatrist will determine what caused the sore.
- Then will remove any dead tissue, clean the wound and apply a bandage.
- Finally, he’ll let you know if you need to adjust your shoes or wear a walking boot, surgical slippers, plantar orthotics, etc.
- Your podiatrist will monitor your situation and make sure you heal properly.
How to prevent diabete effects on your feet
- Control your blood sugar. This is essential for preventing complications of diabetes.
- Avoid “at-home surgeries.” If you have trouble cutting your nails, see your podiatrist.
- Stay away from over-the-counter medicated bandages (e.g., corn patches, salicylic acid for plantar warts, etc.).
- See your podiatrist regularly for proper foot care.
- Never walk barefoot, not even at home. Wear sandals or flip-flops in public places.
- Wear your plantar orthotics.
- Choose shoes that are suitable for the shape of your feet. Specialized stores can help you find proper footwear. Shoe repair shops can stretch leather shoes to accommodate bunions or hammertoes.
- If you experience numbness in your feet, use your hand to check the insides of your shoes before putting them on.
- Wear shoes at all times, especially if you experience numbness in your feet or toes.
- Opt for light-coloured socks. That way you can easily spot blood or pus coming from your feet. Make sure your socks don’t have elastics that could hinder blood circulation.
- Walk or do exercise to promote good circulation and control your blood sugar.
- Stop smoking, as it has a big negative impact on circulation.
- If you are overweight, lose weight to help get your blood sugar under control.
I have a lot of hard skin on the bottom of my feet, but since they don’t hurt, there’s nothing wrong.

Corns occur when there is too much pressure and friction on a specific spot. Blisters can form underneath your corns, leading to sores that are initially hard to see. Patients often discover these sores when remove thick calluses. Many patients with diabetes don’t feel the “alarm signal” indicating that something is wrong, even when a potentially dangerous sore has formed.
And if it was not diabetic effects on your feet?
Some illnesses can cause similar symptoms as diabetes:
- Peripheral vascular disease (on its own)
- Buerger disease
- Charcot-Marie-Tooth disease
- Neuropathy from chemotherapy
- Sciatica
- Tarsal tunnel syndrome
- Kidney disease
- Multiple sclerosis
- Parkinson’s disease