Achilles tendinitis and Achilles tendinosis
A condition characterized by the presence of pain behind the heel originating in the Achilles tendon, the most important tendon in the calf region. The terms tendinitis, tendinosis and tendinopathy refer to the stage and severity of the condition. The Achilles tendon is the most commonly injured tendon among runners.
See the causes See the long term complications See how to relieve yourself at home
Signs and symptoms of Achilles tendinitis
- Pain behind the heel or ankle
- Pain is worse right after rest or when you take your first steps in the morning
- Pain worsens after physical activity
- Pain when walking up or down stairs or inclined surfaces
- Pain worsens when running on uneven terrain
- A lengthening or stretching sensation behind the heel or ankle
- Some patients complain of a burning sensation
- The Achilles tendon may thicken or form a bump
- There may be redness and swelling and the area may feel warm to the touch
What are the causes of Achilles tendinosis
The Achilles tendon is the cord-like tissue located behind the ankle that connects the calf to the heel. With its fibres forming a spiral structure, it’s one of the strongest tendons in the human body and it plays a critical role in movement. In fact, we have the Achilles tendon to thank for the fact that we can stand upright seemingly effortlessly. When we run, the Achilles tendon literally springs into action to propel us forward with ease. It also plays a pivotal role in allowing us to jump. Finally, it greatly helps absorb the impact sustained by the foot.
But this “supertendon” also has its weak points. The blood supply to the Achilles tendon is poor. As a result, it is more prone to injury and heals relatively slowly. When the Achilles tendon suffers repeated and excessive force, microtears can form, leading to inflammation. This stage is referred to as Achilles tendinitis.
Excessive force in the Achilles tendon can be caused by :
- Poor foot mechanics (high arches, flat feet, fallen arches, hyperpronation, leg-length discrepancy, etc.)
- Lack of flexibility in the tendon (insufficient elasticity, genetics, inadequate stretching, etc.)
- Repeated excessive stress (running, speed training, high-impact sports, sports involving jumps or sudden changes in direction of movement, mountain trekking, training on uneven or inclined surfaces, etc.)
- Improper exercise technique
- Inadequate warm-up prior to physical activity
- Inappropriate training program
- Unsuitable footwear
- Being overweight
- Modified gait due to another injury
Progression and consequences of Achilles tendinosis
Given the poor blood supply to the region, if the injury is not treated during the initial stage and if the Achilles tendon continues to bear excessive stress, the fibres in the structure will begin to degenerate.
When the injury enters this chronic degenerative stage, the condition is referred to as Achilles tendinosis or Achilles tendinopathy. If left ignored at this stage, the tendon will weaken further and become susceptible to tearing. In some cases, it may completely rupture.
In cases of chronic excessive tension, calcium deposits may build up in the substance of the tendon or the tendon attachment, forming a bone spur. This process further weakens the tendon and diminishes its flexibility.
How to relieve Achilles tendinitis at home
Alleviating Achilles tendinitis requires stimulating the healing process in the tendon while managing the amount of mechanical stress applied to the area.
1. Rest and relief :
- When pain is present, wear laced shoes with a certain heel like running shoes, as often as possible, even at home.
- Fit your shoes with pharmacy-bought heel cushions.
- Reduce physical activity. While a very mild degree of pain during physical activity is acceptable, the intensity of sports activities should be modified to avoid feeling pain after training.
2. Managing the inflammation :
- In the initial stage, apply ice directly behind the heel 10-15 minutes every hour.
- If the injury is several weeks old, apply a hot and cold treatment by alternating 4 minutes of heat with 2 minutes of ice. Always end with ice.
3. Stretching exercises :
- Warm up your feet when you step out of bed in the morning. Point and lift the toes, make circular movements and stretch your calf muscle with your leg straight while lifting your toes to the ceiling.
- Stretch your calves every evening and after physical activity. Depending on the degree of pain, you can use a wall, step or folded towel as a prop. Hold the position for 30 seconds and repeat 3 times.
- For eccentric strengthening exercises, read about the Alfredson Protocol for Achilles tendon problem.
4. Modifying your exercise program :
- Review your exercise habits and eliminate any aggravating factors.
- Reduce the volume, frequency or intensity of your workouts and take a more gradual approach.
- Reduce physical activity on inclined surfaces.
- Runners should review their technique and include shorter, faster steps. Keep running pace to around 180 steps/minute and reduce the length of your stride. Avoid heavy impacts by paying attention to the way your feet hit the ground. You should strive for a “less noisy” running form. Avoid striking the ground with the heel or inversely, directly on the toes.
Diagnostic of Achilles tendinosis
- X-rays must be conducted on the Achilles tendon to check for calcium deposits and bone spurs. X-rays also make it possible to rule out other causes of heel pain and to assess the alignment of the bones in the foot.
- Ultrasound is an excellent imaging technique and diagnostic tool. It allows the podiatrist to observe the entire tendon, measure its thickness, evaluate the severity of the injury, assess the fibre structure and check for the presence of tears. It also allows us to rule out other conditions affecting the structures surrounding the Achilles tendon.
- To identify whether poor foot alignment or posture may be at fault, a thorough biomechanical exam is essential. This comprehensive evaluation of foot function, gait and posture provides invaluable information. It also includes an analysis of plantar pressure during gait using pressure sensors connected to cameras.
What can my podiatrist do about Achilles tendinitis?
Once the problem has been diagnosed and its potential causes identified, your podiatrist will be able to recommend a personalized treatment plan for your condition.
Some solutions include:
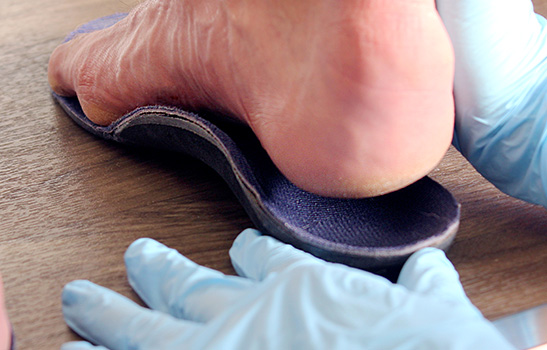
1. Plantar orthotics :
Plantar orthotics help reduce the tension on the Achilles tendon by addressing mechanical problems in the feet. They allow the Achilles tendon to function properly and avoid twisting caused by gait disturbances.
2. Radial shockwave therapy :
Used in chronic cases where patients fail to respond to treatment, this therapy uses the body’s natural capacities to restart the healing cycle, a bit like a time machine. This therapy is successful in 80-90% of chronic cases. Find out more about the radial shockwave therapy.
3. Prescription medication :
Painkillers, muscle relaxants and/or anti-inflammatory drugs may be prescribed.
4. Physical therapy :
- Manipulative therapy
- Cryotherapy and ultrasound
- Taping
- Night socks, splints and walking boots
- Stretching, strengthening and balance exercises
How to prevent Achilles tendinitis?
- Wear adequate footwear.
- Replace running shoes if they wear down or after each 800-1,000 km of use. If your shoes are more lightweight or if you have a larger body mass, you may need to replace your shoes after 500-700 km.
- Take action at the first sign of pain to prevent long-term problems (See “Treating the condition at home”).
- Wear prescribed orthotics daily to help reduce excessive stress on the Achilles tendons.
- If overweight, consider losing weight.
- Warm up well before doing sports or other physical activities.
- After exercising, stretch your calves and the backs of your legs.
- Follow a progressive workout plan, particularly if you run.
- Practice cross-training to vary the types of exercises you do. If running, run on a variety of surfaces (grass, dirt track, etc.).
Cortisone injections are all that's needed to treat Achilles tendinitis.

Quite the opposite! Cortisone injections are strongly discouraged for this condition because they can cause the Achilles tendon to rupture!
And if it was not Achilles tendinosis?
- Achilles bursitis
- Tenosynovitis of the surrounding muscles (fibularis/peroneus muscles, flexor hallucis longus muscle, tibialis posterior muscle)
- Heel bone stress fracture
- Haglund’s deformity
- Synovial cyst
- Posterior ankle impingement
- Fracture of the posterior process of the talus
- Os trigonum syndrome (extra bone in the ankle)
- Referred pain (inflammation of the sciatic nerve or lumbar compression)
- Tumour mass on the heel bone
- Systemic disease (gout, hypercalcemia, lupus, dermatomyositis, rheumatoid arthritis, psoriatic arthritis, ankylosing spondylitis, etc.)